Search
- Page Path
- HOME > Search
Original Article
- Adrenal Gland
- Metabolic Subtyping of Adrenal Tumors: Prospective Multi-Center Cohort Study in Korea
- Eu Jeong Ku, Chaelin Lee, Jaeyoon Shim, Sihoon Lee, Kyoung-Ah Kim, Sang Wan Kim, Yumie Rhee, Hyo-Jeong Kim, Jung Soo Lim, Choon Hee Chung, Sung Wan Chun, Soon-Jib Yoo, Ohk-Hyun Ryu, Ho Chan Cho, A Ram Hong, Chang Ho Ahn, Jung Hee Kim, Man Ho Choi
- Endocrinol Metab. 2021;36(5):1131-1141. Published online October 21, 2021
- DOI: https://doi.org/10.3803/EnM.2021.1149
- 5,114 View
- 209 Download
- 8 Web of Science
- 8 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Conventional diagnostic approaches for adrenal tumors require multi-step processes, including imaging studies and dynamic hormone tests. Therefore, this study aimed to discriminate adrenal tumors from a single blood sample based on the combination of liquid chromatography-mass spectrometry (LC-MS) and machine learning algorithms in serum profiling of adrenal steroids.
Methods
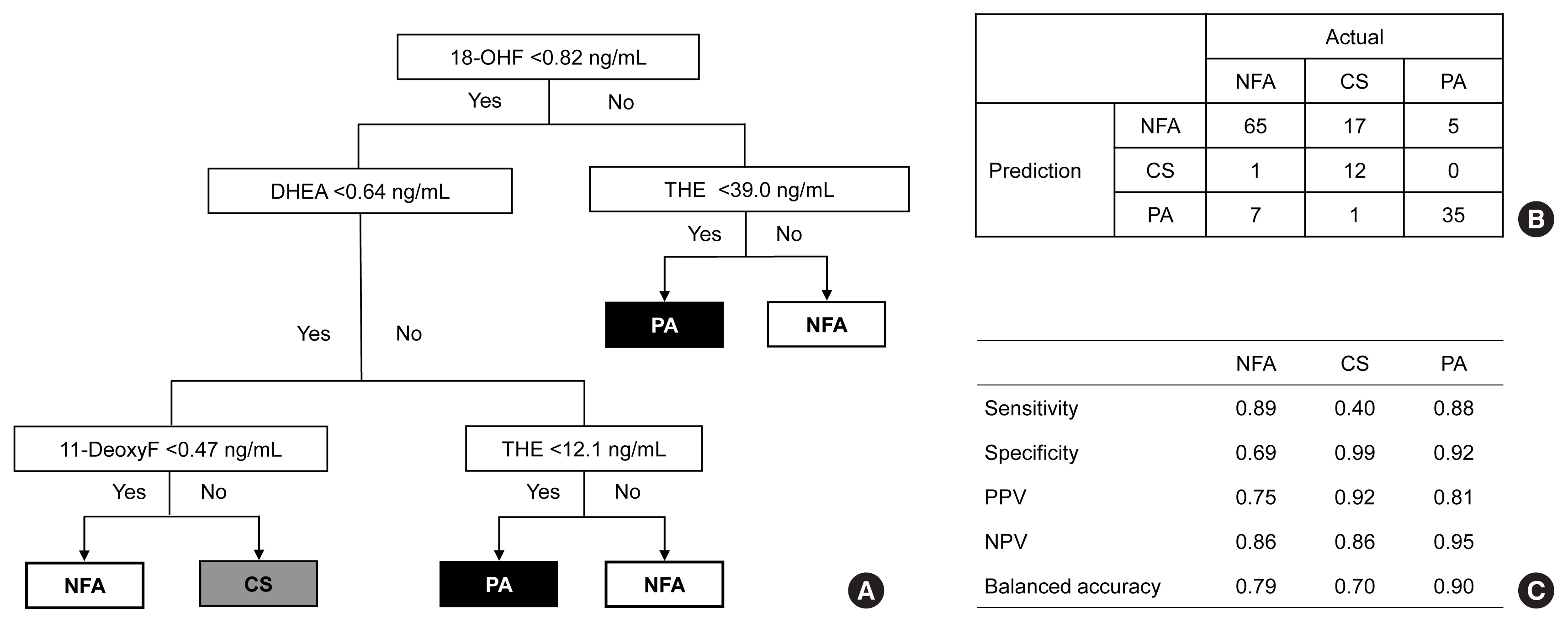
The LC-MS-based steroid profiling was applied to serum samples obtained from patients with nonfunctioning adenoma (NFA, n=73), Cushing’s syndrome (CS, n=30), and primary aldosteronism (PA, n=40) in a prospective multicenter study of adrenal disease. The decision tree (DT), random forest (RF), and extreme gradient boost (XGBoost) were performed to categorize the subtypes of adrenal tumors.
Results
The CS group showed higher serum levels of 11-deoxycortisol than the NFA group, and increased levels of tetrahydrocortisone (THE), 20α-dihydrocortisol, and 6β-hydroxycortisol were found in the PA group. However, the CS group showed lower levels of dehydroepiandrosterone (DHEA) and its sulfate derivative (DHEA-S) than both the NFA and PA groups. Patients with PA expressed higher serum 18-hydroxycortisol and DHEA but lower THE than NFA patients. The balanced accuracies of DT, RF, and XGBoost for classifying each type were 78%, 96%, and 97%, respectively. In receiver operating characteristics (ROC) analysis for CS, XGBoost, and RF showed a significantly greater diagnostic power than the DT. However, in ROC analysis for PA, only RF exhibited better diagnostic performance than DT.
Conclusion
The combination of LC-MS-based steroid profiling with machine learning algorithms could be a promising one-step diagnostic approach for the classification of adrenal tumor subtypes. -
Citations
Citations to this article as recorded by- Treating Primary Aldosteronism-Induced Hypertension: Novel Approaches and Future Outlooks
Nathan Mullen, James Curneen, Padraig T Donlon, Punit Prakash, Irina Bancos, Mark Gurnell, Michael C Dennedy
Endocrine Reviews.2024; 45(1): 125. CrossRef - Steroid profiling in adrenal disease
Danni Mu, Dandan Sun, Xia Qian, Xiaoli Ma, Ling Qiu, Xinqi Cheng, Songlin Yu
Clinica Chimica Acta.2024; 553: 117749. CrossRef - Serum and hair steroid profiles in patients with nonfunctioning pituitary adenoma undergoing surgery: A prospective observational study
Seung Shin Park, Yong Hwy Kim, Ho Kang, Chang Ho Ahn, Dong Jun Byun, Man Ho Choi, Jung Hee Kim
The Journal of Steroid Biochemistry and Molecular Biology.2023; 230: 106276. CrossRef - Recent Updates on the Management of Adrenal Incidentalomas
Seung Shin Park, Jung Hee Kim
Endocrinology and Metabolism.2023; 38(4): 373. CrossRef - LC-MS based simultaneous profiling of adrenal hormones of steroids, catecholamines, and metanephrines
Jongsung Noh, Chaelin Lee, Jung Hee Kim, Seung Woon Myung, Man Ho Choi
Journal of Lipid Research.2023; 64(11): 100453. CrossRef - 2023 Korean Endocrine Society Consensus Guidelines for the Diagnosis and Management of Primary Aldosteronism
Jeonghoon Ha, Jung Hwan Park, Kyoung Jin Kim, Jung Hee Kim, Kyong Yeun Jung, Jeongmin Lee, Jong Han Choi, Seung Hun Lee, Namki Hong, Jung Soo Lim, Byung Kwan Park, Jung-Han Kim, Kyeong Cheon Jung, Jooyoung Cho, Mi-kyung Kim, Choon Hee Chung
Endocrinology and Metabolism.2023; 38(6): 597. CrossRef - Toward Systems-Level Metabolic Analysis in Endocrine Disorders and Cancer
Aliya Lakhani, Da Hyun Kang, Yea Eun Kang, Junyoung O. Park
Endocrinology and Metabolism.2023; 38(6): 619. CrossRef - Prevalence and Characteristics of Adrenal Tumors in an Unselected Screening Population
Ying Jing, Jinbo Hu, Rong Luo, Yun Mao, Zhixiao Luo, Mingjun Zhang, Jun Yang, Ying Song, Zhengping Feng, Zhihong Wang, Qingfeng Cheng, Linqiang Ma, Yi Yang, Li Zhong, Zhipeng Du, Yue Wang, Ting Luo, Wenwen He, Yue Sun, Fajin Lv, Qifu Li, Shumin Yang
Annals of Internal Medicine.2022; 175(10): 1383. CrossRef
- Treating Primary Aldosteronism-Induced Hypertension: Novel Approaches and Future Outlooks

Response
- Diabetes, Obesity and Metabolism
- Association of Protein Z with Prediabetes and Type 2 Diabetes (Endocrinol Metab 2021;36:637-46, Yun-Ui Bae et al.)
- Ji Hong You, Yun-Ui Bae, Ho Chan Cho
- Endocrinol Metab. 2021;36(5):1149-1150. Published online September 16, 2021
- DOI: https://doi.org/10.3803/EnM.2021.502
- [Original]
- 2,668 View
- 76 Download

Original Articles
- Diabetes, Obesity and Metabolism
- Association of Protein Z with Prediabetes and Type 2 Diabetes
- Yun-Ui Bae, Ji Hong You, Nan Hee Cho, Leah Eunjung Kim, Hye Min Shim, Jae-Hyung Park, Ho Chan Cho
- Endocrinol Metab. 2021;36(3):637-646. Published online June 2, 2021
- DOI: https://doi.org/10.3803/EnM.2021.962

- 5,178 View
- 147 Download
- 3 Web of Science
- 5 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Type 2 diabetes mellitus (T2DM) is a progressive metabolic disease. Early detection of prediabetes is important to reduce the risk of T2DM. Some cytokines are known to be associated with T2DM. Therefore, we aimed to identify cytokines as novel biomarkers of glucose dysmetabolism.
Methods
The first stage of the study included 43 subjects (13 subjects with newly diagnosed T2DM, 13 with prediabetes, and 16 with normoglycemia) for cytokine microarray analysis. Blood samples of the subjects were assessed for 310 cytokines to identify potential indicators of prediabetes. The second stage included 142 subjects (36 subjects with T2DM, 35 with prediabetes, and 71 with normoglycemia) to validate the potential cytokines associated with prediabetes.
Results
We identified 41 cytokines that differed by 1.5-fold or more in at least one out of the three comparisons (normoglycemia vs. prediabetes, normoglycemia vs. T2DM, and prediabetes vs. T2DM) among 310 cytokines. Finally, we selected protein Z (PROZ) and validated this finding to determine its association with prediabetes. Plasma PROZ levels were found to be decreased in patients with prediabetes (1,490.32±367.19 pg/mL) and T2DM (1,583.34±465.43 pg/mL) compared to those in subjects with normoglycemia (1,864.07±450.83 pg/mL) (P<0.001). There were significantly negative correlations between PROZ and fasting plasma glucose (P=0.001) and hemoglobin A1c (P=0.010).
Conclusion
PROZ levels were associated with prediabetes and T2DM. We suggest that PROZ may be a promising biomarker for the early detection of prediabetes. Further large-scale studies are needed to evaluate the relationship and mechanism between PROZ and prediabetes and T2DM. -
Citations
Citations to this article as recorded by- On the human health benefits of microalgal phytohormones: An explorative in silico analysis
Angelo Del Mondo, Annamaria Vinaccia, Luigi Pistelli, Christophe Brunet, Clementina Sansone
Computational and Structural Biotechnology Journal.2023; 21: 1092. CrossRef - Role of F-box WD Repeat Domain Containing 7 in Type 1 Diabetes
Sarah W. Mohammed, Zainab M. Qassam, Ekhlass M. Taha, Nameer M. Salih
Ibn AL-Haitham Journal For Pure and Applied Sciences.2023; 36(3): 167. CrossRef - Identification of Protein Z as a Potential Novel Biomarker for the Diagnosis of Prediabetes
Seung-Hoi Koo
Endocrinology and Metabolism.2021; 36(3): 572. CrossRef - Association of Protein Z with Prediabetes and Type 2 Diabetes (Endocrinol Metab 2021;36:637-46, Yun-Ui Bae et al.)
Ji Hong You, Yun-Ui Bae, Ho Chan Cho
Endocrinology and Metabolism.2021; 36(5): 1149. CrossRef - Association of Protein Z with Prediabetes and Type 2 Diabetes (Endocrinol Metab 2021;36:637-46, Yun-Ui Bae et al.)
Tiffany Pascreau, Maia Tchikviladze, Emilie Jolly, Sara Zia-Chahabi, Bertrand Lapergue, Marc Vasse
Endocrinology and Metabolism.2021; 36(5): 1147. CrossRef
- On the human health benefits of microalgal phytohormones: An explorative in silico analysis

- Effects of Alpha-lipoic Acid on SREBP-1c Expression in HepG2 Cells.
- Tae Sung Yun, Ae Kyung Min, Nam Kyung Kim, Mi Kyung Kim, Ho Chan Cho, Hye Soon Kim, Jae Seok Hwang, Seong Yeol Ryu, Keun Gyu Park, In Kyu Lee
- J Korean Endocr Soc. 2008;23(1):27-34. Published online February 1, 2008
- DOI: https://doi.org/10.3803/jkes.2008.23.1.27
- 2,213 View
- 44 Download
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Non-alcoholic fatty liver disease is common in patients with insulin resistance. Sterol regulatory element binding protein-1c (SREBP-1c) is a member of a family of transcription factors that have been recognized as key regulators for lipid accumulation in the liver that activate enzymes involved in the fatty acid biosynthetic pathway. This study was designed to evaluate whether alpha-lipoic acid (ALA) inhibits insulin-stimulated SREBP-1c expression. METHODS: We investigated the effects of ALA on insulin-stimulated SREBP-1c expression in a human hepatoma cell line (HepG2 cells) using Northern and Western blot analysis. We also examined the effect of ALA on the promoter activity of the SREBP-1c gene to examine whether ALA can affect SREBP-1c expression at the transcriptional level. To discern the mechanism by which ALA inhibits SREBP-1c expression, we examined the role of AMP-activated protein kinase (AMPK). RESULTS: Insulin increased the expression of SREBP-1c mRNA and protein in HepG2 cells in a dose depended manner. Co-treatment with ALA inhibited the insulin increased SREBP-1c expression in a dose-dependent manner. ALA also inhibited insulin-stimulated activation of the SREBP-1c promoter activity, indicating that ALA inhibited SREBP-1c expression at the transcriptional level. ALA increased phosphorylation of AMPK in HepG2 cells. Inhibition of the AMPK activity by compound C markedly reversed the inhibitory effects of ALA for insulin-stimulated SREBP-1c expression. These results suggest that ALA-induced suppression of SREBP-1c expression is at least in part mediated via AMPK activation. CONCLUSION: The present study suggests that ALA has an inhibitory effect on insulin-stimulated SREBP-1c expression. Therefore, further studies on the effects of ALA on hepatic steatosis in an animal model need to be performed. -
Citations
Citations to this article as recorded by- Effects of an aqueous extract of purple sweet potato on nonalcoholic fatty liver in high fat/cholesterol-fed mice
You Jin Lee, Yoon Kyoung Yang, You Jin Kim, Oran Kwon
Journal of Nutrition and Health.2015; 48(1): 1. CrossRef - Effects of an aqueous extract of purple sweet potato on nonalcoholic fatty liver in high fat/cholesterol-fed mice
You Jin Lee, Yoon Kyoung Yang, You Jin Kim, Oran Kwon
Journal of Nutrition and Health.2015; 48(1): 1. CrossRef
- Effects of an aqueous extract of purple sweet potato on nonalcoholic fatty liver in high fat/cholesterol-fed mice


 KES
KES

 First
First Prev
Prev



